Endometriosis: Hidden Infertility in Plain Sight
When I was diagnosed twenty years ago, endometriosis was barely talked about, both by professionals and the general public. Now, thanks to celebrities, media figures, social media, and higher rates of diagnosis, endometriosis is getting the attention it deserves. Women across the globe are realizing that the symptoms they’ve suffered through for years, perhaps decades, has a name.
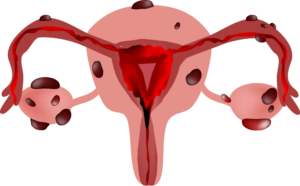
Never heard of endometriosis? Here’s the technical definition: Endometriosis is when endometrial tissue that usually lines your uterus goes rogue and grows outside of the uterus, most commonly found in and on the fallopian tubes, ovaries, bowel, bladder, even stomach.
Before I dive into my story, let’s look at some key points.
Endometriosis Quick Facts:
- It’s estimated that 6-10% of women have endometriosis.
- One of the common causes of infertility.
- Endometriosis cannot be diagnosed via bloodwork or ultrasound.
- Diagnosis is usually delayed by an average of six years!
- There are no physical attributes associated; women of all weights and statures are susceptible.
The cause of endometriosis is still unknown, as is the cure. Currently, the two most common treatments are laparoscopic surgery to remove the tissue and/or taking birth control pills to control estrogen levels (my experience with these is written below).
Now, here’s the tricky part with diagnosis, some patients exhibit symptoms, others do not, hence why this condition is “hidden in plain sight.” I personally did not have any symptoms when I was first diagnosed.
Common Endometriosis Symptoms Include:
- Heavy and/or painful periods.
- Pain during intercourse or bowel movements.
- Bloating and cramping.
- Infertility.

How Does Endometriosis Affect Fertility:
- Endometriosis is estrogen-dominant, meaning the body has a surplus of estrogen and therefore can cause a hormonal imbalance.
- Endometrial tissue grows outside the uterus, in and around the fallopian tubes, ovaries, bowel, bladder, stomach, etc. This can impede both travel and implantation of the egg.
- Adhesions, which I personally have a few of, and scar tissue can damage ovaries and fallopian tubes.
- It’s estimated that 30-50% of endometriosis patients incur infertility.
My Endometriosis Diagnosis
I did not have heavy periods or pain, so my endometriosis probably went undiagnosed for years. This all changed when I had a rupturing cyst that required laparoscopic surgery. Low and behold, the doctor found severe endometriosis—everywhere, including both fallopian tubes and ovaries. Yet neither the bloodwork nor the many ultrasounds detected it.
Interestingly enough, when I was diagnosed with PCOS six months prior, the endocrinologist said he assumed I had endometriosis, which he told me seemed to go hand in hand with PCOS, in his experience at least. This was twenty years ago, so this may have changed, or it still might be relevant. Either way, his assumption was correct.

The doctor subsequently removed part of an ovary and an entire fallopian tube due to both the cyst and the overgrowth of endometriosis. What I didn’t realize was removing the endometriosis causes scar tissue that can also be painful and impede on your fertility, and that endometriosis never goes away—it continues to grow. As mentioned above, there are studies that show birth control pills slow the growth of endometriosis, unfortunately, they did not help in my case.
About ten years after my official diagnosis, I started getting endometriosis symptoms in the form of very (probably an understatement) heavy periods. And, of course, infertility.
Flash Forward to my Fertility Journey
I knew we would need help with our fertility journey, mainly for my PCOS. What I didn’t expect was to find another massive cyst that would have to be removed before we started any fertility procedures. So, off to the hospital for laparoscopy number two, where my doctor finds severe endometriosis everywhere—again. On a scale of one to four (four being most severe), I was at a four, and this was after they had removed the existing endometriosis years prior. The doctor also found that my only remaining fallopian tube was pinched from scar tissue and the new round of endo growth, so an egg would have trouble traveling through it.
Of course, this was after we’d spent too much valuable time on both Clomid and Letrozole, wishfully hoping for a positive during every cycle, only unbeknownst to me, that single fallopian tube was practically out of working order. And it was a good thing we hadn’t jumped into the first line of procedures, an IUI, because again, my road was partially blocked which would lower my IUI success rate.
This meant our best possible fertility treatment would be IVF, where the fertility specialist bypasses the fallopian tubes completely. Which honestly, was the way we were leaning anyway after losing so much time with the medications above.
Once that surgery was over, I knew time was of the essence before the endometriosis grew back, so the very next day (I kid you not!), I was scheduling my appointment with Dr. Lin at the Reproductive Fertility Center in Irvine. This PCOS, Endometriosis, and cyst-prone mama thought it was going to be a rough ride, spoiler alert: I got pregnant.
Final Thoughts on Endometriosis
If you have heavy periods, painful periods, or unexplained infertility, endometriosis might be something to look deeper into. The unfortunate part is that there are no easy tests, and exploratory surgery may be needed for diagnosis. But, ruling this in or out and treating the condition will help direct your fertility treatment.
There are some tests you can have done before you start your fertility journey, and while they won’t diagnose endometriosis, they will check off some other boxes, and you can work via the process of elimination. These include, blood work, HSG (hysterosalpingogram)(checks for fallopian tube blockage), ultrasound, SIS (saline infusion sonohysterography)(checks uterine cavity).
I hope the community continues to bring light to endometriosis, both for a diagnosis’s sake and treatment’s sake.
Endometriosis: Hidden Infertility in Plain Sight is a true story written by an RFC patient.



